The 13th Osstell ISQ Annual Symposium will gather an exciting line-up of international speakers, featuring Dr. Tara Aghaloo (USA), Dr. William Martin (USA), Dr. Stephen T Chen (Australia), Dr. Kyle Stanley (USA) and moderator Dr. Marcus Dagnelid (Sweden).
5 reasons to attend the 2021 Osstell ISQ Symposium
[fa icon="calendar'] Jun 21, 2021 2:23:48 PM / by Osstell posted in loading protocol, immediate restoration, isq, implant loading, primary stability, Osstell scientific symposium, digital workflow, immediate loading, rfa, secondary stability, osseointegration, implant healing, implant stability, risk patient, healing time, implant placement
Why measuring Osstell ISQ on abutment level can help you achieve predictable outcomes
[fa icon="calendar'] Mar 10, 2021 7:47:54 PM / by Osstell posted in loading protocol, immediate restoration, isq, implant loading, primary stability, immediate loading, rfa, osseointegration, implant healing, implant stability, healing time, SmartPegs
Treating osteoporotic patients: a review by Dr. Tara Aghaloo
[fa icon="calendar'] Jul 8, 2020 1:34:08 PM / by Osstell posted in isq, risk patient, healing time
Loading Protocols for Daily Implantology: Interview with Dr Zita Gomes
[fa icon="calendar'] Jun 30, 2020 2:27:59 PM / by Osstell posted in isq, insertion torque, immediate loading, implant stability, CBCT
Dr. Raquel Zita Gomes DMD, PG, MSc, PhD, Oral Surgeon, University Prof. will present and discuss the loading protocols (delayed, early, immediate) in modern oral implantology, and create guidelines for daily decisions in this webinar.
Dr. Jeff Ganeles answers your clinical questions
[fa icon="calendar'] Oct 25, 2019 5:55:36 PM / by Osstell posted in loading protocol, isq, implant loading, primary stability, EAO, immediate loading, secondary stability, implant stability, risk patient, implant complication, healing time, implant placement
Ask the expert! Dr. Barry Levin answers your questions.
[fa icon="calendar'] Oct 24, 2019 9:18:05 AM / by Osstell posted in loading protocol, isq, implant loading, primary stability, EAO, immediate loading, secondary stability, implant stability, risk patient, implant complication, healing time, implant placement
When To Immediately Load an Immediate Implant
[fa icon="calendar'] May 7, 2019 6:41:21 PM / by Barry P. Levin, DMD posted in immediate restoration, isq, primary stability, Immediate Implant Insertion Torque, immediate loading, implant stability, implant placement
Ask the experts!
[fa icon="calendar'] Nov 22, 2018 8:43:00 AM / by Osstell posted in loading protocol, isq, implant loading, primary stability, EAO, immediate loading, secondary stability, implant stability, risk patient, implant complication, healing time, implant placement
Clinicians from all over the world participated to Osstell Scientific Symposium at EAO Congress 2018 in Vienna, on October 11th.
How to Determine the Degree of Osseointegration Before Final Restoration
[fa icon="calendar'] Nov 14, 2018 8:28:00 AM / by Osstell posted in isq, primary stability, rfa, secondary stability, osseointegration, implant stability, healing time
Have you ever placed an implant in an augmented bone site and added another few months of healing time just to be on the safe side?
The Importance of Implant Stability in Successful Dental Implant Therapy
[fa icon="calendar'] Sep 16, 2018 5:23:00 PM / by Osstell posted in isq, primary stability, secondary stability, osseointegration, implant stability
It has long been recognized in the dental implant literature that implant stability is a critical factor in predictable treatment outcomes. Both primary stability (mechanical stability) and stability prior to provisionalization or restoration of the implant should be considered in the individual treatment plan. The secondary (aka biological stability) will indicate the level of osseointegration when compared to the initial primary stability (mechanical stability) at placement of the implant. There are other factors, of course, to be considered but there is little disagreement in the literature that implant stability is key.
Primary and Secondary Stability: What is Important and What Don’t We Know
[fa icon="calendar'] Jul 3, 2018 2:25:05 PM / by Barry P. Levin, DMD posted in isq, primary stability, Immediate Implant Insertion Torque, insertion torque, secondary stability, osseointegration, implant stability, healing time
Physiologic healing after implant placement varies from patient to patient and site to site. Surgeons must find balance between mechanical stability and avoiding excessive trauma to alveolar bone, especially the cortical bone found at the alveolar crest. The two measures of quantifying primary stability are insertion torque volume (ITV) and resonance frequency analysis (RFA). Implant stability quotient or ISQ is a value used to determine stability via RFA.
Why secondary stability is crucial for successful implant treatments.
[fa icon="calendar'] Apr 5, 2018 9:52:00 AM / by Osstell posted in isq, primary stability, immediate loading, rfa, secondary stability, osseointegration, implant stability
Primary and secondary stability is a much discussed topic. Which one should a clinician aim for to achieve successful implant treatments? We met with Dr. Stephen Jacobs after his lecture at the AO Annual Meeting about primary and secondary implant stability to clarify things.
Could you explain the difference between primary and secondary stability?
How I determine loading protocol and timing of restoration
[fa icon="calendar'] Mar 5, 2018 10:17:16 AM / by Dr. Rachel Schallhorn posted in loading protocol, isq, implant loading, immediate loading, implant planning, osseointegration
Measuring ISQ has become a critical component in my implant treatment, as it provides objective information about the stability of the implants I place. Based upon the initial implant stability or ISQ value, I determine the loading protocol and timing of restoration (immediate, early, delayed).
How to Confidently Reduce Treatment Time? [With Case Report]
[fa icon="calendar'] Feb 9, 2018 8:36:56 AM / by Charles D. Schlesinger posted in loading protocol, isq, primary stability, insertion torque, immediate loading, rfa, healing abutment, case report, osseointegration
I have been placing dental implants since 1998 and as most of you, I have seen many advances in the field of dentistry that make implant dentistry safer and more predictable. The biggest boon to treatment absolutely has to be the advent of CBCT technology. This has made the surgical phase of treatment more predictable and safer for the patient.
Meet Dr. Michael Norton [video]
[fa icon="calendar'] Jan 30, 2018 1:09:33 PM / by Jonas Ehinger posted in loading protocol, isq, primary stability, insertion torque, rfa, secondary stability
Dr. Michael Norton talks about Osstell ISQ and RFA in his practice. Dr. Norton has been using Osstell for many years and has found value in having the information it provides to him about his patients. In addition, Dr. Norton is just completing his term of office as President of the Academy of Osseointegration which will hold its 2018 Annual Meeting in Los Angeles February 28th through March 3rd. We and Dr. Norton welcome your comments and questions on his thoughts.
Thoughts and reflections from Osstell Scientific Symposium at EAO 2017 in Madrid
[fa icon="calendar'] Dec 1, 2017 10:48:15 AM / by Jonas Ehinger posted in isq, grafted bone, regenerative protocols, Osstell scientific symposium, EAO, insertion torque, digital workflow, osstellconnect, immediate loading, rfa
Clinicians from all over the world participated to Osstell Scientific Symposium at EAO Congress in Madrid, on October 5th. This year’s symposium featured Dr Steven Eckert, Dr Giorgio Tabanella and Dr Luis Cuadrado.
We sat down with moderator Dr Marcus Dagnelid, from Gothenburg, Sweden, and collected his thoughts and reflections of the scientific content of the symposium on this blog post. Ask questions to Dr Marcus Dagnelid in the comments at the bottom of the page!
Dr Marcus Dagnelid, moderator at Osstell Scientific Symposium, DDS, Board Certified Prosthodontist
The Correlation Between Immediate Implant Insertion Torque and Implant Stability Quotient
[fa icon="calendar'] Nov 23, 2017 2:25:21 PM / by Barry P. Levin, DMD posted in immediate restoration, isq, implant loading, primary stability, Immediate Implant Insertion Torque
I was curious about the correlation between immediate insertion torque (IT) and ISQ and wanted to study it in my practice. This is a study I conducted and it was published in IJPRD recently. The study protocol and findings are posted here for you to read and comment on.
Thanks,
Barry Levin
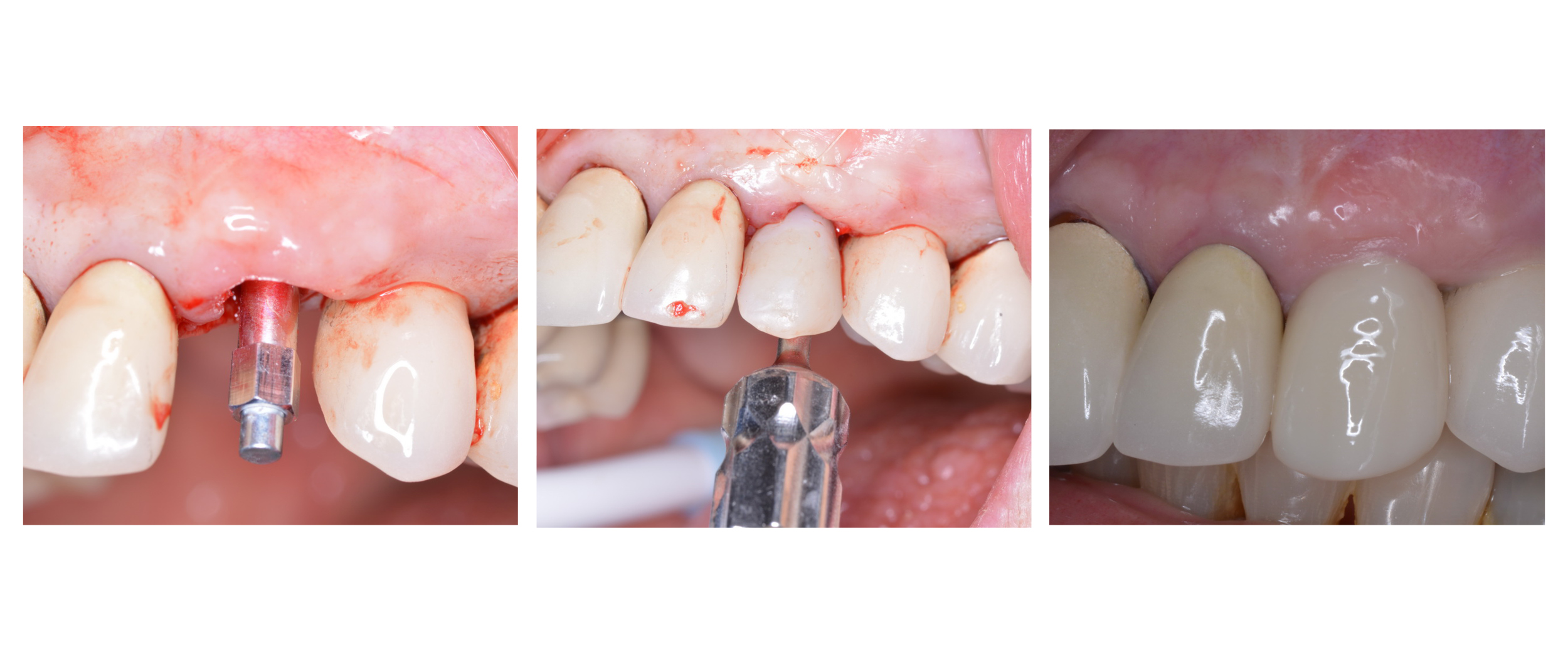
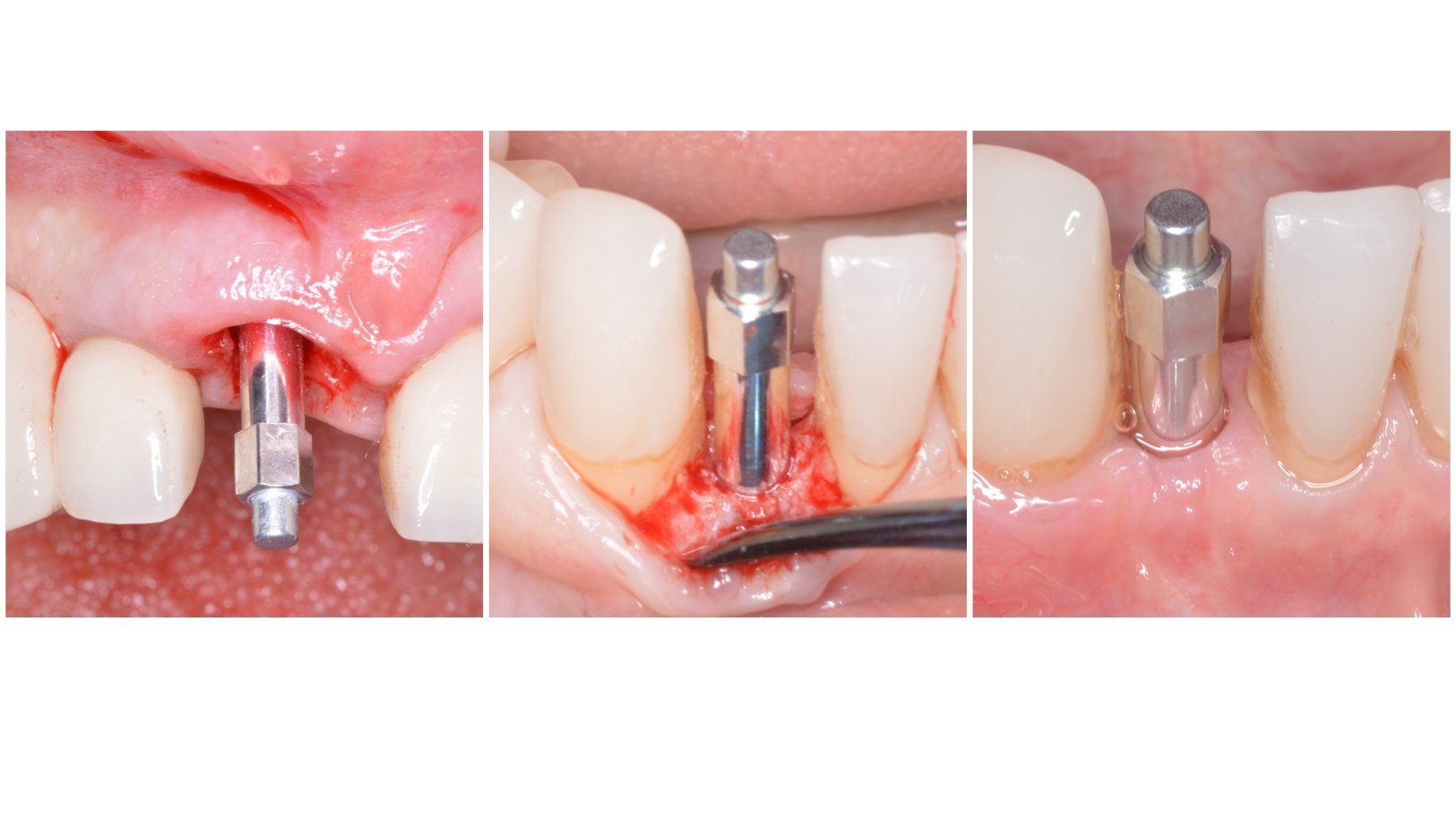
How Progressive Loading Solved a critical Implant Case.
[fa icon="calendar'] Sep 27, 2017 5:27:31 PM / by Francisco Teixeira Barbosa posted in loading protocol, immediate restoration, progressive loading, isq, implant loading
Every day we do a lot of things based on our intuition. We make decisions based on our own or others experience.
We do not need science to help us in our daily life, and we don't have a clear indicator that shows us if our decision is the best.
Decisions based on practical experience is our way of life.
But when it comes to our profession as dentists, we do, or at least we should, evidence-based dentistry for...almost every treatment we perform.
As the title of this article says, I´m going to present a case about "progressive loading."
Yes, I know, progressive loading is supported by few clinical studies (Rotter 1996, Appleton 2005, Ghoveizi 2013), but -and here comes the interesting part- the rationale behind this concept makes sense from a clinical and biological point of view.
















.jpg)